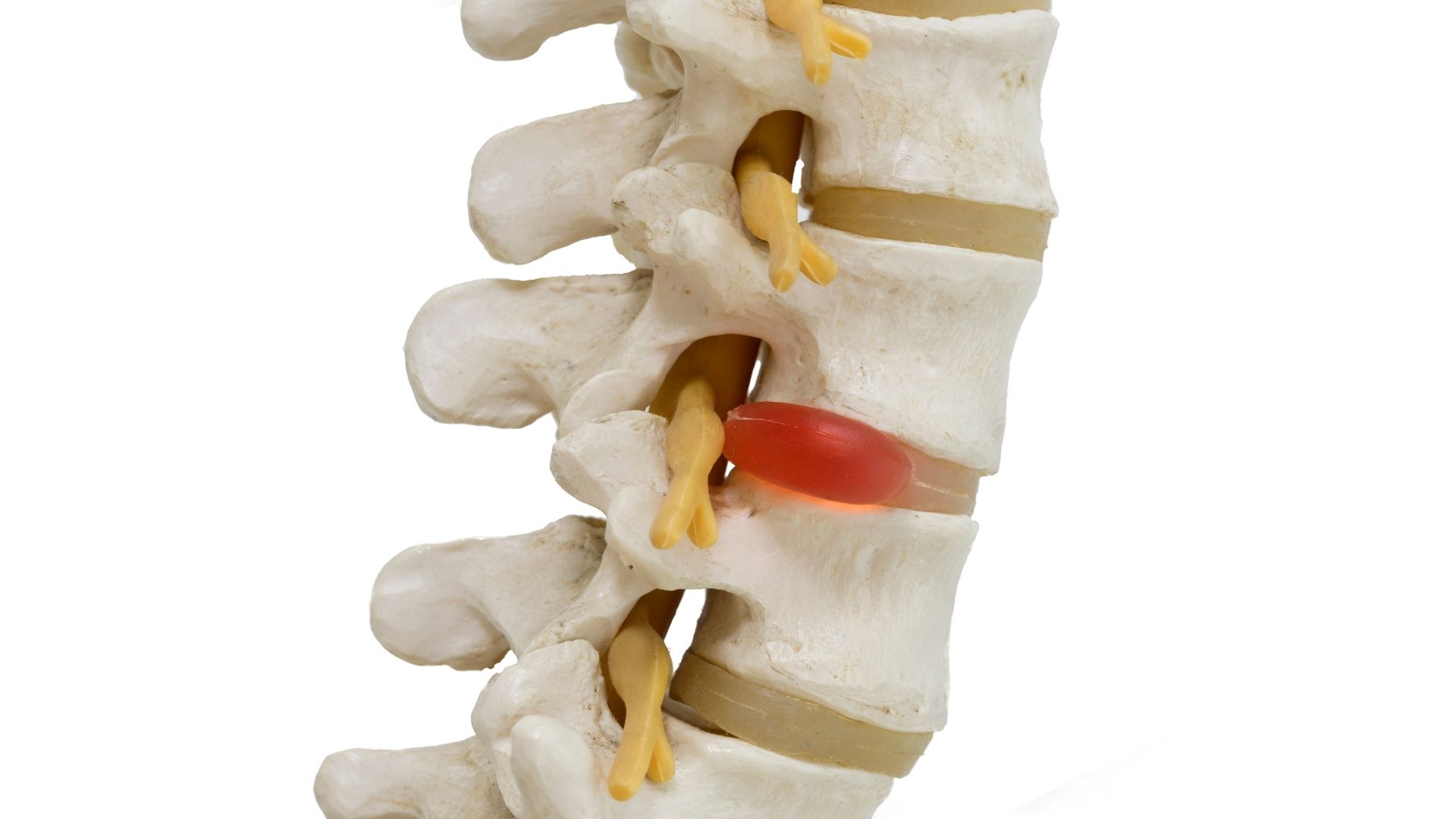
A discectomy is a surgical procedure that removes a herniated disc from the spine. Herniated discs typically occur in individuals between the ages of 30 to 50 years old and is twice as common in males, compared to females[i].
In this article, we will describe what a discectomy is and why it is performed, in greater detail. Additionally, we will discuss how physical therapy can help manage post-operative pain and improve function and mobility following a discectomy.
What is a Discectomy?
A discectomy is a surgical procedure that might be considered to address issues caused by a herniated disc pressing on a nerve root extending from the spinal cord, or the spinal cord itself, including pain, weakness and sensory changes.
Disc degeneration is a natural result of aging and can occur from normal wear and tear on the spine making a disc more susceptible to herniation. Individuals with a herniated disc present with symptoms of numbness and weakness along with lower back pain. If conservative treatments, like medications or rest, are unable to alleviate symptoms this procedure is considered.
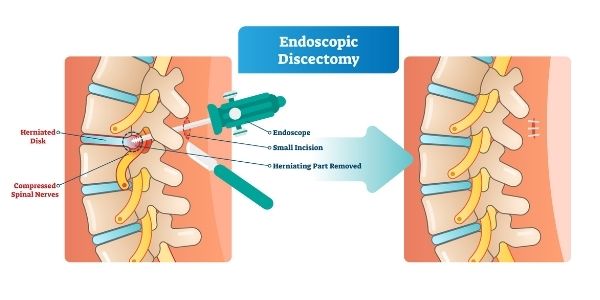
Discectomies can be performed through several different surgical techniques, but minimally invasive procedures have been shown to reduce the length of hospital stays and post-operative pain[ii]. However, your doctor will select the surgical technique that is most appropriate for you.
During a minimally invasive procedure, the affected disc is removed while leaving the surrounding bones, muscles, and soft tissues decreasing the risk of post-operative instability compared to alternative approaches like an open discectomy[iii].
Anatomy of the Spine
The spine is composed of 24 separate bones, called vertebrae, which are stacked on top of one another. These vertebrae are connected to each other by intervertebral discs, which function as shock absorbers and help to maintain adequate space for spinal nerves to exit the vertebral column.
Intervertebral discs are composed of the annulus fibrosus and nucleus pulposus. The annulus fibrosus is the tough outer layer of the disc and the nucleus pulpous is the jelly-like interior of the disc. The shock absorbing function of the intervertebral disc comes primarily from the jelly-like qualities of the nucleus pulposus, while the annulus fibrosis functions to keep the nucleus pulposus centered within the disc.
A disc herniation occurs when the nucleus pulposus bulges out of the disc, due to a tear or rupture in the annulus fibrosis. If this bulging of the nucleus places pressure on the spinal cord or spinal nerves, pain, weakness or sensory changes may be experienced. To reduce the pressure being placed on these structures and address these symptoms, the herniated disc can be removed by performing a discectomy.
Herniated Disc Symptoms
The goal of a discectomy is to remove the herniated disc that is placing pressure on the spinal cord or nerve roots to help alleviate symptoms. A herniated disc can occur anywhere in the spine. Consequently, discectomies can be performed in the cervical, thoracic or lumbar regions of the spine. Nerve compression in the cervical spine can produce sharp pain in the neck, or between the shoulder blades, that can radiate down the arm and may also be associated with numbness and tingling.
If nerve compression occurs in the lumbar spine, these same symptoms occur in the lower extremity and radiate down the legs. A discectomy is considered if conservative treatments are unsuccessful in managing pain, to the point where activities of daily living are negatively impacted.
Post Discectomy Surgery Pain Management
Following a discectomy, pain management is a priority to help patients return to activities of daily living. Medications and ice will be used to manage both pain and swelling. Additionally, activities that involve any strenuous activity, such as lifting, bending or twisting, must be modified or avoided altogether.
Proper incisional care is required to ensure the incision heals properly and to reduce the risk of infection or other complications. Physical therapy should be started as soon as possible after surgery to promote mobility and protect against future injury.
How Long Does It Take to Recover from Discectomy Surgery?
Physical therapy treatment plans will be individually tailored to meet patients’ needs. In general, treatment plans will work to address strength, flexibility and mobility impairments. A 2002 study showed that 12-week post-operative exercise programs following a discectomy improve pain, disability, quality of life and spinal function[iv].
In addition, proper education regarding safe movements in a tolerable range is an essential part of post-operative treatment plan. Range of motion exercises will help to restore movement within a safe limit.
Musculature imbalances that may occur following surgery will be addressed through the prescription of specific resistance exercises to target these impairments. Once proper stabilization is achieved, exercises will be progressed accordingly. Working together with the clinician is essential to properly advance exercises while restoring movement and returning to activities of daily living.
At Propel Physiotherapy, our team of highly trained and experienced clinicians are skilled in the treatment of a variety of complex conditions. Physical therapy plays an integral role in the management of pain and restoration of function post-operatively. If you have recently undergone a discectomy, book an appointment with one of our therapists so they can help you return to your everyday life.
References
[i] Jordan J, Konstantinou K, O’Dowd J. Herniated lumbar disc. BMJ Clin Evid. 2011;2011:1118. Published 2011 Jun 28.
[ii] Joaquim, Andrei Fernandes, Botelho, Ricardo Vieira, Mudo, Marcelo Luis, Almeida, Antonio Silvinato de, & Bernardo, Wanderley Marques. (2018). Lumbar herniated disc – endoscopic discectomy treatment. Revista da Associação Médica Brasileira, 64(5), 397-407. https://doi.org/10.1590/1806-9282.64.05.397
[iii] Xinhua Li, Yingchao Han, Zhi Di, Jian Cui, Jie Pan, MingJie Yang, Guixin Sun, Jun Tan, Lijun Li, Percutaneous endoscopic lumbar discectomy for lumbar disc herniation, Journal of Clinical Neuroscience, Volume 33,
2016, Pages 19-27,ISSN 0967-5868, https://doi.org/10.1016/j.jocn.2016.01.043.
[iv] Gulsah ogutluler ozkara, , Merih ozgen, , Emre ozkara, , Onur Armagan, , Ali Arslantas, Metin Ant Atasoy, Effectiveness of Physical Therapy and Rehabilitation Programs Starting Immediately After Lumbar Disc Surgery. Turk Neurosurg 2015, Vol: 25, No: 3, 372-379. 10.5137/1019-5149.JTN.8440-13.0
Written by
OUR LOCATIONS
FOLLOW US!
OUR SERVICES
Last Updated on July 27, 2022 by Propel Physiotherapy