Gait impairment is common in people with Parkinson’s disease (PD), affecting mobility, independence and increasing falls risk. Over the past few decades, research and clinical studies supporting the effects of using music clinically in rehabilitation have been developed and replicated. One of the most powerful and well-documented elements of music on non-music functions is rhythm. In this blog, we will look at how rhythmic auditory stimulation can help improve walking and function for those living with PD.
Parkinson’s disease (PD) is the second most common neurodegenerative disorder after Alzheimer’s disease.[i] The disease is caused by loss of cells in the brain that produce dopamine, a neurotransmitter that acts to plan and control bodily movements. The characteristic motor symptoms of the disease include slowness of movement (bradykinesia), rigidity, tremor and postural instability.[ii] All of these symptoms can greatly impact gait and function.
The motor impairments in PD cause various gait abnormalities including difficulty regulating stride length, reduced velocity, ‘freezing’ of gait and increased cadence or step rate.[iii] The consequence of this includes increased morbidity and mortality rate and decreased quality of life.[iv]
Due to the areas affected in PD, planning, processing, and sequencing of walking is greatly affected. Spatiotemporal (relating to distance and time) components of gait including step length, stride length, cadence, velocity and single limb support time are all altered. An external stimulus such as auditory cuing can help to recalibrate timing mechanisms and improve rhythm of movement.
What is Rhythmic Auditory Stimulation?
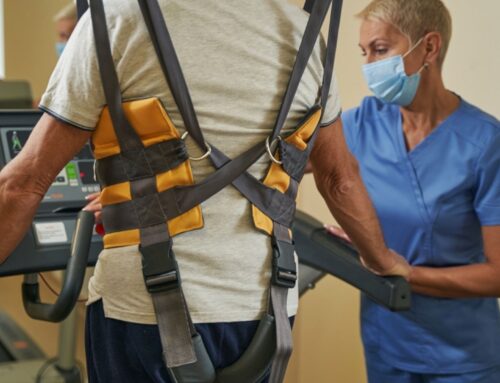
Rhythmic auditory stimulation uses sound and often treadmill training to simulate external cues and facilitate a normal gait pattern. This can be done through counting, a metronome or music to help provide a feedback system for walking. This stimulus has been found to improve gait parameters such as step length, velocity and overall gait quality.
A systematic review of over 20 randomized controlled trials found that gait training and auditory cuing are effective in improving gait abnormalities and kinematics in PD clients.[v] Another study found that rhythmic auditory stimulation reduced the number of falls in PD clients and improved gait parameters such as velocity and stride length.[vi]
Propel Physiotherapy offers highly trained and specific treatment plans including body weight supported treadmill training and rhythmic auditory stimulation to enhance functional goals. Rhythmic auditory stimulation is a holistic and versatile form of therapy that moves beyond words and taps into something inherent in all of us; music and rhythm.
Parkinson’s Exercise Classes
We also offer the PWR!Moves classes to specifically meet the exercise needs of people with PD. This skill-based training program was designed to maintain or restore skills that can deteriorate or interfere with everyday movements. The program helps to target all the motor symptoms of PD using functional skill training.
Propel Physiotherapy is now offering Parkinson’s exercise classes virtually every Monday from 2-3 PM with PWR!Moves® Certified Therapist Shriya Maharaj. The PWR!Moves® program is one more important tool to help Propel Physiotherapy meet our goal of helping our clients maintain or restore skills that help them live life optimally.
You may also enjoy reading: Parkinson’s Exercise Classes Virtual
Physiotherapy Management of Parkinson’s Disease
For people with PD, the things we do every day automatically or habitually – such as swinging our arms when we walk, getting out of bed, and getting up off the floor – become more difficult. The progressive neurological disorder can be a devastating and life-changing diagnosis. The good news is that evidence suggests that exercise can slow the progression. Let our experienced therapists help assess, design and plan a targeted exercise program that is right for you.
You may also enjoy reading: Physiotherapy Helps Symptoms of Parkinson’s Disease
References
[i] Wu XY, Han LH, Zhang JH, Luo S, Hu JW, Sun K. The influence of physical activity, sedentary behavior on health-related quality of life among the general population of children and adolescents: A systematic review. PLoS One. 2017;12(11):e0187668. Published 2017 Nov 9. doi:10.1371/journal.pone.0187668
[i] https://www150.statcan.gc.ca/n1/pub/82-003-x/2014011/article/14112-eng.htm
[ii] https://www.parkinson.ca/about-parkinsons/symptoms/
[iv] https://movementdisorders.onlinelibrary.wiley.com/doi/epdf/10.1002/mds.870110213
[iv] https://www.sciencedirect.com/science/article/pii/S0149763413001930
[iv] ibid.
[v] Rutz DG, Benninger DH. Physical therapy for freezing of gait and gait impairments in Parkinson‘s disease: a systematic review. PM&R. 2020 Jan 29.
[vi]https://pubmed.ncbi.nlm.nih.gov/30033755/#:~:text=Conclusion%3A%3A%20RAS%20training%20significantly,as%20velocity%20and%20stride%20length.
Written by